New study shows effectiveness of shorter TB treatment
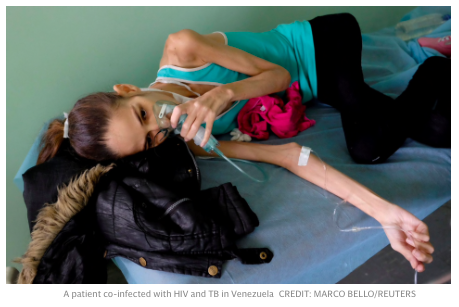 A new study provides vital evidence that a nine-month treatment regime for one of the more serious forms of tuberculosis is just as effective
A new study provides vital evidence that a nine-month treatment regime for one of the more serious forms of tuberculosis is just as effective
as the standard programme which can take up to two years.
Patients with multi-drug resistant TB (MDR-TB) have to take a cocktail of toxic drugs, whose side effects include kidney problems, psychological problems and deafness, as well as an initial course course of painful daily injections.
The standard treatment time is 20 to 24 months and the regimen is expensive and patients find it hard to stick to.
Last year the World Health Organization (WHO) changed its guidance to recommend a shorter treatment regimen but admitted that there was limited evidence of its effectiveness.
Now, the first ever randomised control trial of a TB regimen has found that the shorter nine- to 11-month course is as effective as the 20- to 24-month treatment course.
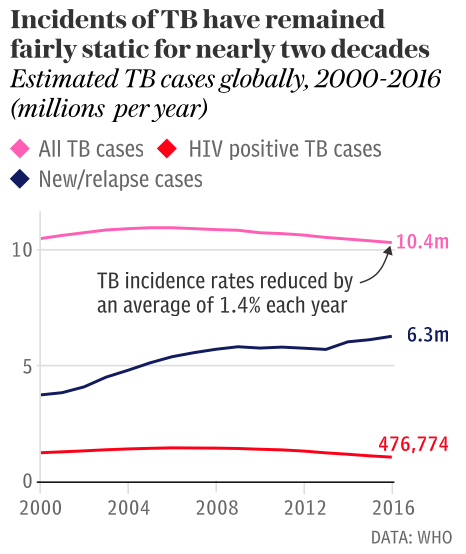
Finding effective treatments for TB is vital to ending the epidemic. The latest figures from the World Health Organization (WHO) show that 10 million people were infected with TB in 2017, and 1.6million of those people died. The world is not on course to hit WHO targets to slash the number of new cases of the disease by 90 per cent and deaths by 95 per cent between 2015 and 2035.
In the global study, published in the New England Journal of Medicine, 424 patients at seven sites in Vietnam, Mongolia, South Africa and Ethiopia were randomly assigned to a treatment programme, with around a third of patients going on the long regimen and two thirds going on the short regimen.
The study found that the nine-to-11 month programme was just as effective as the longer version. The results showed that 78.8 per cent of patients on the shorter course were still free of TB two and a half years after the end of the treatment, compared to 79.9 per cent on the longer programme.
The study also found that patients who were HIV positive had just as good outcomes on the short programme as on the long programme.

Researchers from the Liverpool School of Tropical Medicine are currently looking at the cost effectiveness of the shorter treatment period.
Paula Fujiwara, scientific director of the International Union Against Tuberculosis and Lung Disease, said the trial was good news in that it provided vital evidence of the short programme’s effectiveness.
“Analysis of the cost effectiveness is ongoing but the initial idea is that of course the shorter programme will be cheaper. When you take medicine for nine months instead of 24 months the costs will go down. One of the key goals of the [WHO] Stop TB strategy is that patients will avoid catastrophic costs and we hope that the analysis will show this,” she said.
The study found that the long regime actually performed a lot better under clinical trial conditions than it usually does – the longer regimen has a 50 per cent effectiveness rate usually, compared to nearly 80 per cent in the trial.
However, in observational studies – where patients are treated in real world conditions – the shorter regimen performed just as well as in the randomised control trial, suggesting that the shorter regimen is actually more effective than the longer one.
“During the trial we create a very supportive environment to ensure patients stay on treatment. This is not feasible in the real world,” said ID Rusen, co-author of the study.
The researchers are also conducting a second trial which includes the use of a new TB drug, bedaquiline, which cuts out the need for painful injections. Researchers hope that this will prove as effective as previous studies.
The study also showed that there was a slightly higher death rate among patients taking the shorter treatment compared to those on the longer treatment – 6.4 per cent compared to 8.5 per cent.
“When we looked more closely there was nothing obvious happening that meant a higher death rate for those on the shorter treatment regimen. MDR-TB is a very serious disease and death is not uncommon,” said Dr Rusen.
By: Anne Gulland
Source: https://www.telegraph.co.uk/news/0/new-study-shows-effectiveness-shorter-tb-treatment/









